In-Office Testing and Treatments for Dry Eye
Dry Eye Testing
Diagnosis of dry eye can be accomplished through either a comprehensive eye examination or a problem-focused medical visit. Information obtained through patient history and our dry eye questionnaire can help gauge the severity of your symptoms while a microscopic view of your eyes will be used to determine the clinical level of your condition.
Further testing will be performed at your initial dry eye evaluation and monitored at regular visits to ensure improvement of symptoms and ocular health. We begin by performing a tear film osmolarity reading with our TearLab instrument. This painless test helps to quantify the severity of your dry eye and can be used at future visits to monitor the results of your treatment.
Our doctors will evaluate your ocular health, lid structure, and blink dynamics by using a microscope. Specially dyed drops may be used to observe the quantity and quality of your tears and highlight changes made to the surface of the eye caused by poor tear flow or insufficient tears.
Based on the findings, a treatment plan will be created for you and may include the use of over-the-counter or prescription eye drops, lifestyle or contact lens changes, nutritional supplements, and at-home treatments or in-office procedures.
In-Office Dry Eye Treatments
iLux
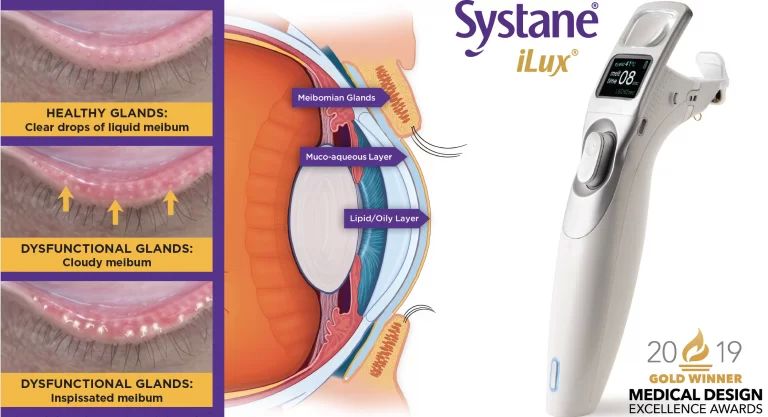
The iLux is our most advanced piece of equipment for treating meibomian gland dysfunction (MGD) in the office. The meibomian glands lie within the eyelid and release the lipid layer of the tear film. This oil layer (also known as meibum) helps to prevent the tears from evaporating too quickly, resulting in dry eye symptoms.
In healthy eyes, meibum should easily flow out of the meibomian glands like water and onto the surface of the eye. In meibomian gland dysfunction, the glands become clogged with thickened meibum which must be forced out like toothpaste! If this oil is not properly removed, the glands may become infected (causing styes), inflamed (causing a chalazion), or permanently damaged (causing severe and irreversible dryness).
If MGD is left untreated, the meibomian glands can begin to atrophy. Once severe atrophy has taken place, they will no longer function. This results in chronic dry eye symptoms. Since there is currently no treatment available once they reach this stage, obtaining relief becomes very difficult.
Studies show that about 86% of dry eye sufferers have signs of MGD, and these signs can be present in patients who don’t even have symptoms of a dry eye yet! In order to keep the oil flowing freely and the meibomian glands healthy and functional, we need to melt the meibum and unclog the meibomian glands. At-home treatments such as warm compresses and lid scrubs can help, but not as efficiently as the iLux.
The iLux is a handheld instrument that uses thermal pulsations (localized, light-based, heated compressions) to clear any meibomian gland obstructions and melt the meibum so that it flows freely. This helps treat and prevent dry eye symptoms, but more importantly, it works to maintain the integrity of the meibomian glands to protect against future irreversible damage.
The iLux procedure takes about 8-12 minutes to perform and is performed on both upper and lower lids. Its effect usually lasts for over a year but may need to be repeated during the year depending on the severity of your MGD.
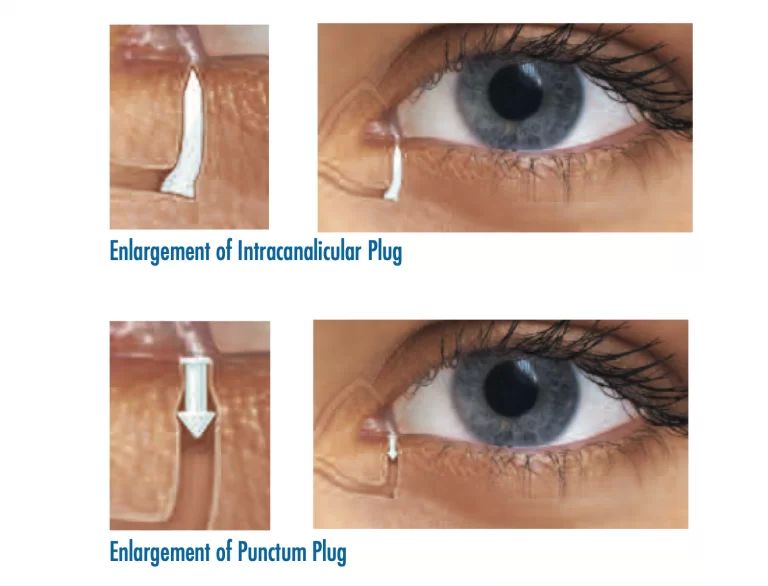
Punctal Plugs
In order to keep natural tears in the eyes longer, we can block off the tear ducts (the puncta) in order to slow their drainage. This can be accomplished in-office by using tiny collagen or silicone plugs, called punctal plugs.
If you are a candidate for this procedure, our doctors will begin by inserting temporary plugs made of collagen that will dissolve within a few weeks. If this treatment is successful, we can then insert silicone plugs which are designed to last for years, but can still be removed if necessary. We can also refer to an ophthalmologist to have the puncta permanently closed through surgery, if necessary.
Punctal plugs are easily inserted in-office using a numbing drop, tweezers (or pre-loaded applicator), and the slit lamp (microscope). Patients with severe ocular inflammation may not be a good candidate for this procedure and may require additional treatment prior to, or in place of, punctual plugs.
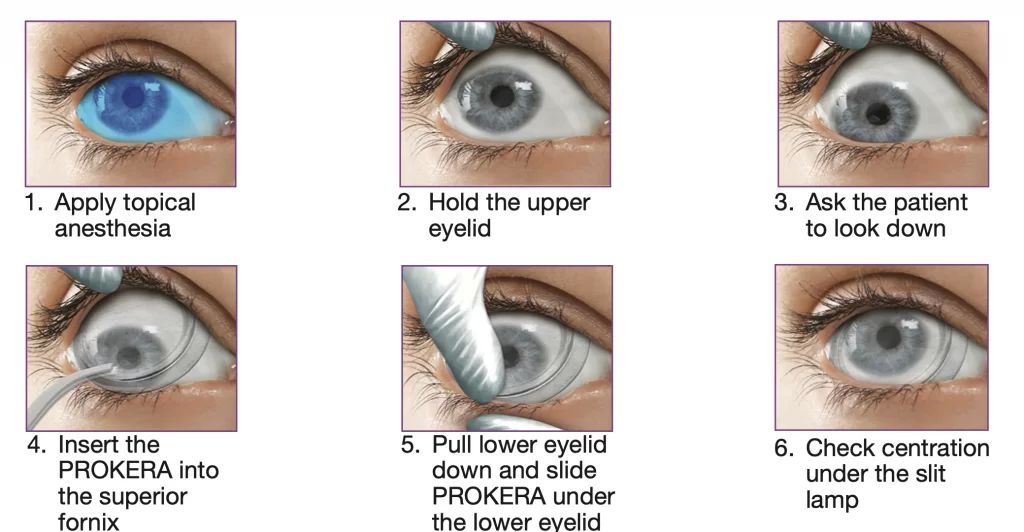
Prokera
PROKERA is a biologic bandage contact lens used in patients with moderate to severe dry eye, or other types of corneal disorders. The lens features an amniotic membrane tissue that provides natural anti-inflammatory and anti-scarring properties to promote faster and more effective ocular surface healing than other treatments can provide.
The PROKERA lens is easily inserted in-office and left in place for 5 days. You will then return to the office to have the lens removed and inserted into the fellow eye for another 5 days. Ideally, this will prevent dry eye symptoms from occurring for the next 5-7 months, at which point another PROKERA insertion is recommended (subsequent treatment may require fewer days of wear).
Scleral Lenses
Another lens-based treatment available for dry eye (and other corneal conditions) is a scleral lens. These are custom-designed, rigid contact lenses with a large diameter that vaults over the cornea and rests on the white surface of the eye (the sclera). This creates a small pool of tears between the lens surface and the cornea which works to provide moisture and symptom relief.
Prescription Medications
In addition to the above in-office treatments we offer, our doctors are also able to prescribe medications to help increase the production of tears and/or decrease existing inflammation that causes dryness. These medications are incredibly effective and have historically been the gold standard in quickly managing dry eye signs and symptoms.
Depending on the severity of your disease, you may only be prescribed a short-term medication such as Eysuvis, or you may require daily maintenance medications such as Restasis, Xiidra, or Cequa. It might also be necessary to use a combination of other prescription drops or ointments, oral medications, eyelid cleaners, or nutritional supplements to properly maintain your dry eye symptoms.
To find out which of these in-office treatments might work best for your dry eye, call our office to schedule an appointment today!